A new daily pill could help individuals maintain weight loss after completing injection treatments, a study suggests.
Researchers indicate that switching to orforglipron offers an “effective approach” for sustaining weight loss, especially for those not wishing to remain on jabs.
Experts also note the drug is “significantly cheaper to manufacture” than current options like Wegovy and Mounjaro.
Orforglipron, a GLP-1 agonist, works by lowering blood sugar levels, slowing food digestion and reducing appetite.
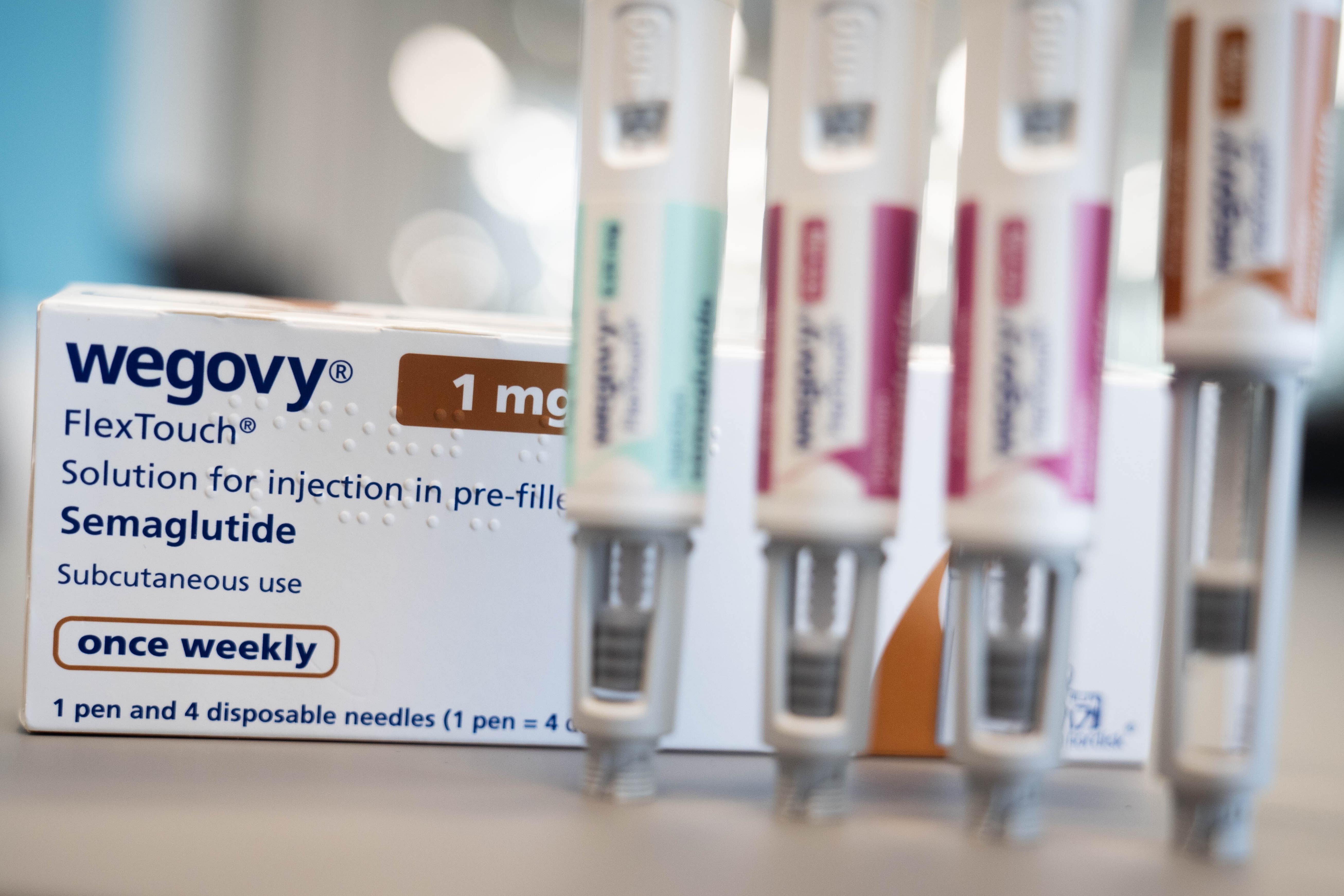
However, instead of being injected, it is taken once-a-day as a tablet.
The drug – made by Eli Lily – is not yet licensed in the UK, but was approved by the Food and Drug Administration in the US last month.
A trial involved 376 people in the US who had already been on tirzepatide or semaglutide – used for weight loss on the NHS under the brand names Mounjaro and Wegovy – for 72 weeks.
Over a year, patients either took orforglipron every day or a placebo.
Researchers found that among those who had been on tirzepatide, patients who moved onto orforglipron maintained 74.7 per cent of their weight loss after a year compared with 49.2 per cent taking the placebo.
Some 79.3 per cent of former semaglutide users also maintained their weight loss compared to 37.6 per cent in the placebo group.
Previous studies have found that people on weight loss jabs are likely to regain weight.
Researchers suggest that transitioning onto orforglipron “may be an effective approach for maintaining weight loss for those who do not continue injectable therapy”.
Reacting to the findings, which have been published in Nature Medicine, Dr Marie Spreckley, research programme manager at the University of Cambridge, said: “One of the most valuable aspects of this study is that it reflects a highly realistic clinical scenario.
“Many people do not want to remain on injectable therapy indefinitely due to treatment burden, convenience, travel, storage requirements, cost, or personal preference.
“The possibility of transitioning to an oral therapy while maintaining a substantial proportion of the previously achieved weight reduction could therefore represent an important additional option within longer-term obesity care pathways.”
Dr Simon Cork, senior lecturer in physiology at Anglia Ruskin University (ARU) highlighted that while patients lost more weight using injectable drugs, they are expensive.
“This limits their long-term applicability both for private purchasers and the NHS,” he said.
“Newer, oral medications are significantly cheaper to manufacture, but do not tend to produce the same level of weight loss seen with injectable medications.”
Dr Cork added that more research is needed with a larger group of patients, but said the findings point to “a potential future for how patients with obesity are treated, and how the success of weight loss can be maintained”.